Tourniquet conversion: when and how to change tourniquet to bandage

Entry
The information in the article is a compilation of material from American medical specialists with extensive experience in business trips to Iraq, Afghanistan, and Africa. Further, the word "conversion" is equivalent to the word "replacement" and is left to reduce the risk of distorting the meaning conveyed by the authors. Please be understanding.
Turnstile conversion
In the current situation of mobilization, in addition to the blind production of copies of tools like a tourniquet, it is necessary to analyze, systematize and convey to users the practical experience of working with these tools, at least in text.
Unfortunately, the number of cases has increased when, already in the hospital, the victim loses a limb after prolonged exposure to a tourniquet-tourniquet or due to an error in application. Therefore, in addition to the time limit on the duration of the impact of the tourniquet tourniquet, you need to remember the phrase "turnstile conversion".
Tourniquet conversion is the replacement of an already applied tourniquet with a pressure bandage or hemostatic agents. The tourniquet conversion is carried out in stages with the control of bleeding and the imposition of an additional safety tourniquet higher than the one already used.
Actions to save the victim take precedence over diagnosis until the first pause in the situation.
conversion procedure. Abstract:
• Replacement of the active tourniquet should be done as soon as possible, but no later than 2 hours after the initial tourniquet application.
• Conversion of a tourniquet placed 2-6 hours ago is considered relatively safe because there is no scientifically determined limit beyond which a tourniquet causes irreparable harm.
• Tourniquets placed more than 6 hours ago are not subject to conversion in the field and are removed only in a hospital setting.
Turnstile "Plus-1"
The authors introduce the concept of the Plus-1 turnstile. In fact, this is a new additional safety turnstile, ready to work in case of failure of the main one, since the turnstiles are subject to the destructive effects of the environment and significant wear during use.
Procedure:
1. Apply the Plus-1 tourniquet and loosen the first tourniquet.
2. If there is no bleeding from the wound, leave both tourniquets in place, not tightened, bandage the wound.
3. If there is bleeding, apply a hemostatic agent.
4. If the hemostatic did not help, the first tourniquet (the one that has already been tightened) is moved as close as possible to the wound and pulled up. The Plus-1 tourniquet stays in place, fully weakened, and is used as a backup if the main one fails to control the bleeding.
examples:

Figure 1. Model patient with a single tourniquet placed on the upper thigh. The tourniquet is placed high and tight in the proximal position due to the need for immediate control of bleeding during the Care Under Fire phase. Diagnostics (examination of the wound) is carried out at the stage of "Field Assistance" (TFC, Tactical Field Care). Tourniquet remains visible and marked with application time
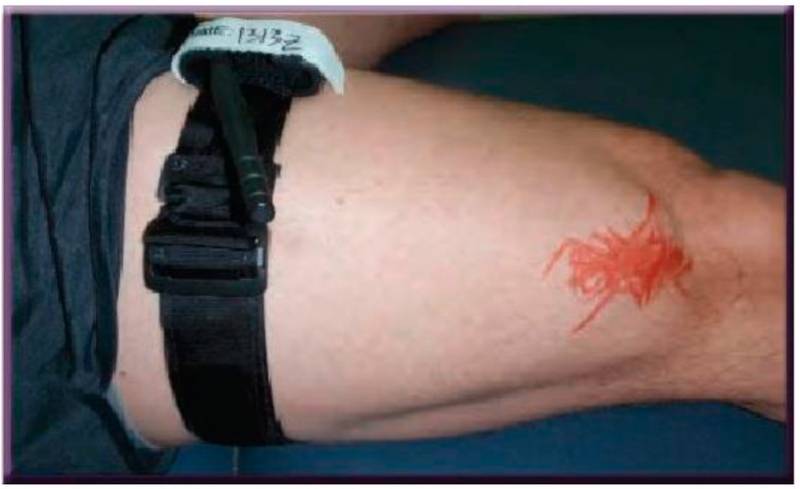
Figure 2. For educational purposes, the same tourniquet is shown on a bare leg. The simulated injury is the distal femur (red marker). No active bleeding noted and no distal pulse
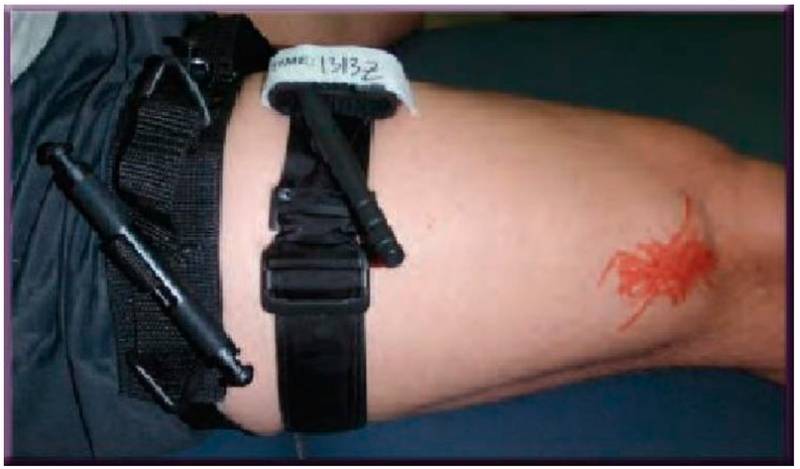
Figure 3. The next step is to place the Plus-1 tourniquet proximal to the first. Turnstile "Plus-1" does not tighten
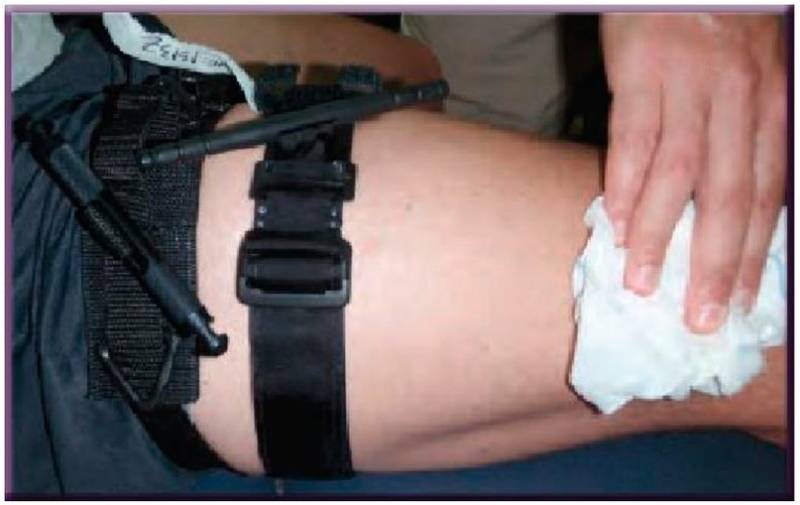
Figure 4. Attempted application of a hemostatic agent. The wound is examined, the original tourniquet is opened, and a hemostatic agent is applied. After that, it is necessary to hold it under pressure for 3-5 minutes.
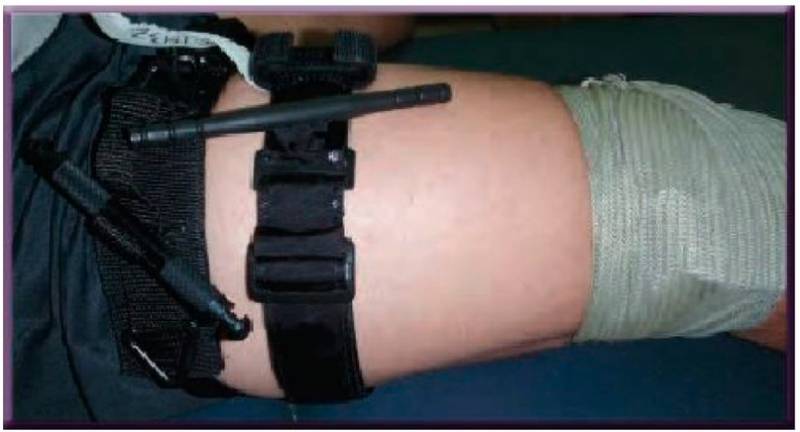
Figure 5. The hemostatic agent is protected by a pressure dressing. If no further bleeding is noted, both the original and the Plus-1 tourniquet remain fully weakened in place.
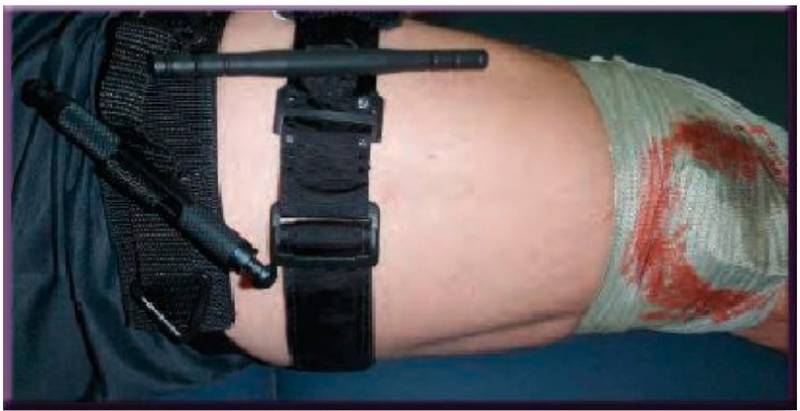
Figure 6 Conversion failed and wound is bleeding through hemostatic agent/dressing
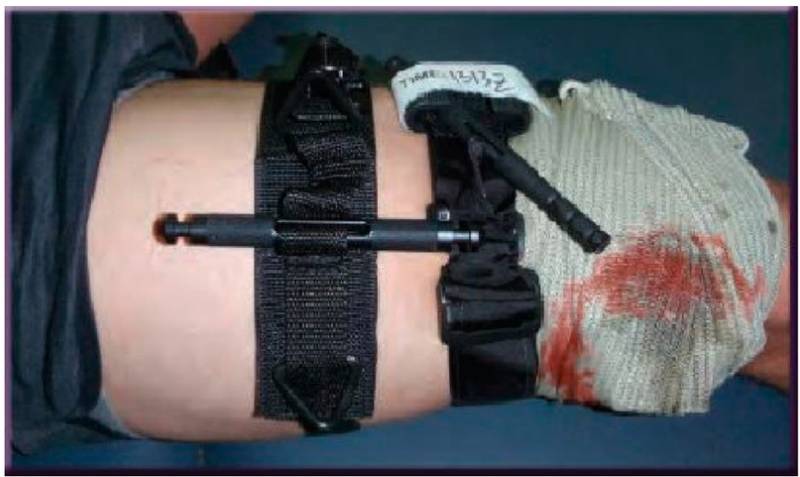
Figure 7. The first tourniquet is moved as close to the wound as possible and pulled up. The turnstile "Plus-1" remains in place completely weakened. If bleeding recurs, the Plus-1 tourniquet is already in place and ready for quick tightening
Keep the hemostatic under pressure for 3-5 minutes. If no further bleeding is noted, leave both loose tourniquets in place and bandage the wound. If hemostatic agents fail to control bleeding, tighten the first tourniquet as far as possible distally to control bleeding. Verify that there is no distal pulse. Leave the Plus-1 harness loose.
When should the turnstile not be replaced?
• At amputation. The tourniquet is placed 5–10 cm above the amputation, avoiding the joints, but proximal enough to prevent bleeding.
• Tourniquet conversion is prohibited unless direct observation of the casualty is possible. For example, if he is wrapped in a rescue blanket or other material to prevent hypothermia.
• Conversion is prohibited for casualties in a state of shock. This problem was documented as early as 1945. Wolf and Adkins reported on a severely injured patient with tachycardia and hypotension who lost approximately 100 ml of blood during a tourniquet reset procedure. He showed immediate clinical signs of exacerbation of shock and a drop in systolic blood pressure to 80 mm Hg. Art. If hemorrhagic shock is suspected, resuscitation should be initiated before tourniquet conversion is attempted.
Tourniquets should not be loosened periodically, because the wound also periodically begins to bleed, which can lead to fatal blood loss. The tourniquet should only be loosened during the conversion procedure.
Among other things, regardless of hemodynamics and considerations of tissue preservation, tourniquets are very painful to use. Any intervention that reduces pain in the wounded is important from a medical and psychological point of view. Pain can cause tachycardia, and improved pain control can help reduce the incidence of PTSD.
Conclusion
Tourniquets are an important tool at the initial stage of limb injuries, which are accompanied by massive bleeding. However, the use of a tourniquet can lead to significant complications later.
Ideally, rapid change to hemostatics and/or standard wound dressing should be performed by qualified and trained medical personnel, but everyone should know the basic information.
Information